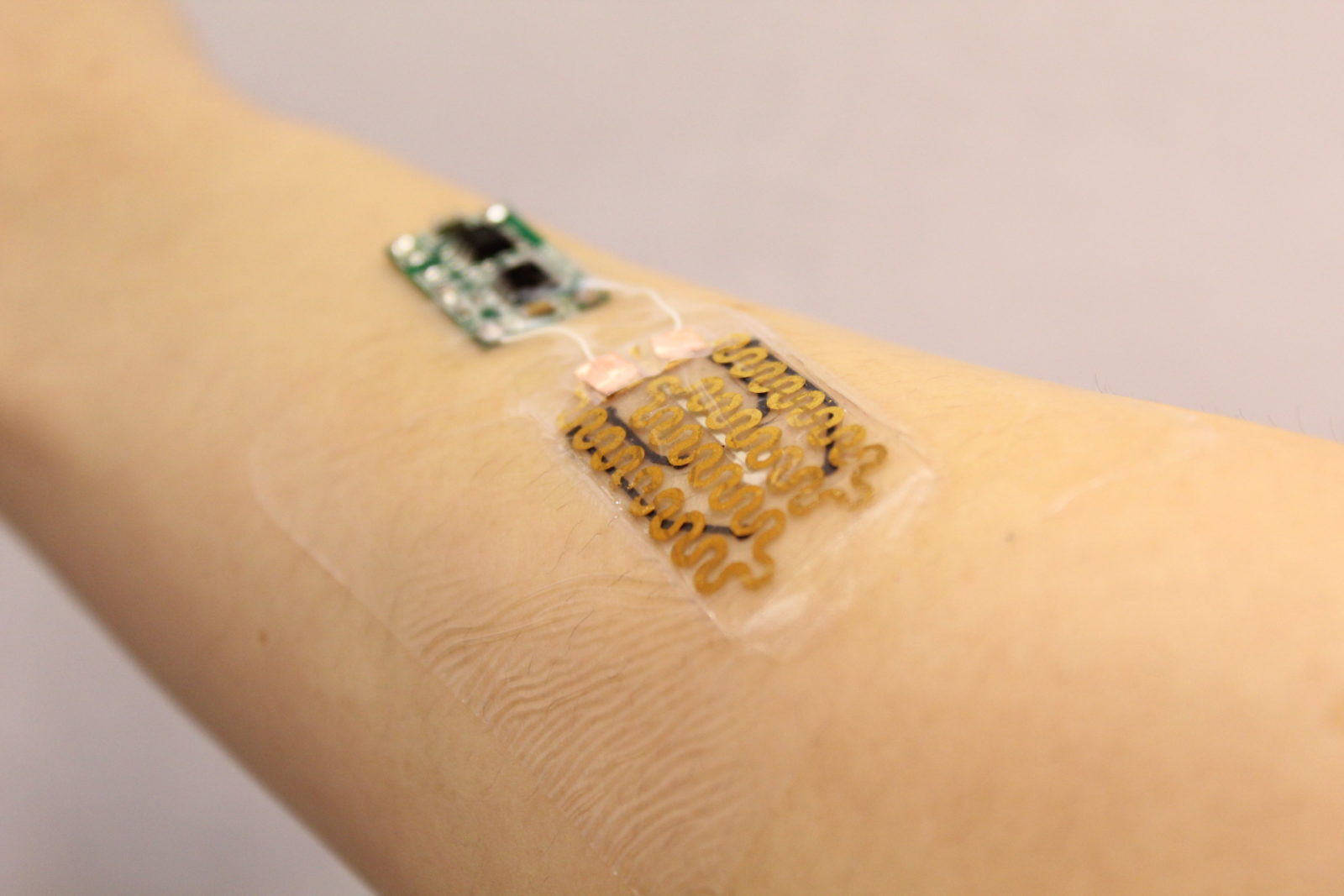
A team of researchers from Tuft University in Massachusetts has developed a prototype of a “Smart Bandage”, which is designed to actively monitor the condition of chronic wounds and deliver appropriate drug treatments to improve the chances of healing.
The prototype is still in the testing phase. A study, published in the journal Small, says that the this Smart Bandage would enable the doctors to monitor their patient’s condition more actively, which not only is superior over the traditionally passive methods but can also be used for patients with sensitive conditions like diabetes or obesity.
How it Works
The smart bandage is a flexible strip with all the tech goodies inside it, like its central processor, sensors, Bluetooth, a heater and a drug dispenser.
It will be able to sense how fast the wound is healing, also detecting the temperature, pH, and level of inflammation in and around the wound. If it senses any changes in the temperature or pH levels it can automatically dispense an appropriate quantity of drugs to treat the wound which, of course, a doctor can program to administer if certain conditions are detected.
The paper states
A stimuli‐responsive drug releasing system comprising of a hydro-gel loaded with thermo‐responsive drug carriers and an electronically controlled flexible heater is also integrated into the wound dressing to release the drugs on‐demand.
The bandage can provide real-time status updates about the wound via Bluetooth.
In order to make the bandage cheaper and reusable, the research team used 3D-printed materials and detachable layers.

Why Do We Need Smart Bandages?
According to lead researcher Pooria Mostafalu “The wound environment is dynamic, but their healing rate can be enhanced by administration of therapies at the right time.”
ALSO READ
Asus VivoWatch BP Brings Medical Grade Blood Pressure Monitoring & Stress Index
With an increase in diseases like obesity and diabetes, it’s becoming more and more difficult to treat the patient or wounds that heal at an unpredictable rate, making it a challenge for physicians to identify and treat the wounds to avoid infections.
Sameer Sonkusale, the co-author of the study, said
Chronic wounds are one of the leading causes of amputations outside of war settings. We believe smart flexible bio-electronics technology has the potential to improve the health outcome of these wounds.
“It has applications in bed sores, burns, and surgical wounds,” he said. “It can reduce complications from infections and reduce the number of amputations. And all of this is possible because your bandage intervened appropriately at the right time to make your wounds heal faster,” he continued.
This closed loop ‘sense-then-respond’ bandage is probably the first of its kind.
These futuristic patches haven’t yet made it to the market and there is still a lot of room for development and testing, as the researchers are going to test these on animals first.